The Independence at Home Act S.3130
The Independence At Home Act – S.3130 is bipartisan legislation to convert Independence at Home – team-based house calls for frail older adults — into a permanent national Medicare program. It was introduced in the Senate on July 6, 2016 by Senators Markey, Cornyn, Bennet and Portman. Six more co-sponsors have joined the bill: Brown, Cassidy, Gillibrand, King, Klobuchar, and Stabenow. Conversion into a national program is now supported by over 80 organizations, advocates and caregivers.
What is Independence at Home? It is an evidence-based healthcare delivery model that uses interdisciplinary teams of medical and social services professionals to provide primary care in the home to seriously ill and disabled older patients. It is also called ‘home-based primary care’ or ‘home care medicine,’ or ‘house calls.’ It is not hospice care or home health agency nursing care. Independence at Home (IAH) has been proven to deliver high quality primary clinical care and excellent patient experience, while significantly lowering overall Medicare costs.
Independence At Home Act and The University of Arizona
The University of Arizona is a recognized leader in home care medicine.
Conversion of IAH to a national program would enable the University of Arizona to sustain and expand its cutting-edge programs and claim its position as the national academic leader in this emerging, highly innovative field. Mindy J. Fain, MD, the Anne & Alden Hart Professor of Medicine and co-Director of the University of Arizona Center on Aging, is the President of the American Academy of Home Care Medicine (AAHCM). This is the professional home care medicine organization representing over 1000 clinicians, organizations, and industry partners.
Arizona and the University of Arizona are ideally suited to lead the field. The opportunities in research, education and clinical care are enormous. As the focus of care transitions from the hospital/clinic to the home and community, innovative academic-industry and community partnerships are required to fully realize the potential.
The Origins of the Independence At Home Act
Backed by a large body of evidence, the IAH Medicare Demonstration Pilot Program was launched in 2012 to test the effectiveness of home-based primary care for frail older adults. It compared IAH to usual care, and any savings were shared between Medicare and the practices. The 24/7, team-based clinical-financial model required practices to meet rigorous quality standards in order to participate in the shared savings. After two years, this pilot program has been hailed as the most successful Medicare Demonstration project to date.
Here are the results: IAH dramatically improved care for nearly 10,000 Medicare patients in 17 pilot practices across the U.S., and yielded total Medicare savings of $35M during the first two years – an average of ~$1,000-$3,000 per beneficiary.
The cost savings — a reduction in total Medicare costs by up to 30% — were due to better access to care, coordinated chronic care management, fewer unnecessary ER visits and hospitalizations, and improved advance care planning.
It is estimated that 1-2 million Medicare patients with severe chronic illness and disability could benefit from access to IAH practices. These patients currently suffer poor quality care, and are among our most costly. A national IAH program would bring and estimated $10 to $15 billion in savings over the next 10 years. In Arizona, 36,400 older adults would benefit from this program – and the number is growing.
Several Key Components Make IAH Successful
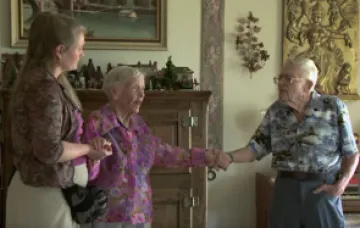
IAH is designed to provide appropriate level of care for a carefully targeted group of the most complex, high cost beneficiaries – only the sickest and most frail Medicare beneficiaries are eligible to participate. The shared savings design incentivizes practices to take high-need and high cost patients, and reward only those practices with demonstrated success. The design prevents unnecessary hospitalization and misuse of medications, and discourages overuse of services. IAH has rigorous quality standards.
Enrollment is voluntary, and patient/family satisfaction is tied directly to shared savings. The required team-based model means increased coordination of care and higher quality. IAH requires that the practice provides access to care 24/7, uses electronic health record technology, and offers in-home visits within 48 hours of hospital or ED discharge, including medication reconciliation.
For details on the IAH legislation, please visit this website.
Next Steps: Make IAH Accessible to Frail Older Adults in Arizona and Across the Country
Why is passage of S.3130, the Independence at Home Act, so important?
The champion bipartisan Senators’ press release in 2016 quoted Dr. Fain saying, “IAH successfully fills a critical gap in health care for our frail and elderly that few programs have been able to achieve. In the process, it improves patient satisfaction and health outcomes, while simultaneously saving money. We are delighted that a bipartisan group of U.S. Senators introduced this legislation.” (S.3130)
IAH is a targeted, proven, and bipartisan success. However, it is limited to the 17 pilot project demonstration practices, and it is not available across the country — yet.
The shared savings model of IAH provides the necessary financial infrastructure to sustain and grow home care medicine programs. Without access to shared savings, home care medicine programs across the country struggle to survive as the current fee-for-service reimbursement doesn’t match home care clinical and operational delivery costs. Unless the practice is part of a larger integrated delivery system (e.g., accountable care organization, or VA) which benefits from the overall cost savings, it can’t survive without philanthropic, extramural or foundational support.
As a result, an estimated 1-2 million vulnerable older adults (36,000 in Arizona) are unable to access care and benefit from this high quality program — and Arizona and the nation lose millions in cost savings.
Without the ability to sustain and grow home care medicine programs in Arizona, the University of Arizona — a national leader in the field — struggles too, and we are unable to benefit from the vast opportunities in research and interprofessional education.
The University of Arizona and the Future of Home Care Medicine
With passage of IAH, the University of Arizona will be able to sustain and expand our current comprehensive home care medicine education and research portfolio which includes innovative practices in Tucson and Arizona’s rural border regions; interprofessional team training in home care medicine; and partnerships with clinician researchers across campus on a range of clinical and policy issues. Stakeholder engagement is an integral part of all home care medicine activities and extends the reach and potential impact. Federal funding opportunities and private foundations are actively engaged in supporting research. For example, the John A. Hartford Foundation recently awarded $1.5M to scale home-based medical care into the mainstream of U.S. Health Care (Co-PI: Fain).
A sample of activities/awards that we are positioned to engage in/receive includes:
- Lead state-of-the-art scientific research, including private-public partnership, academic-community engagement, and industry collaboration to create the next generation of bedside and remote diagnostics and technologies to support seriously ill adults at home.
- Lead interprofessional education and clinical care about home care medicine
- Collaborate with Arizona Telemedicine Program and Banner Health’s iCARE in partnership with the mobile clinical team
- Lead interprofessional education to build the home care medicine workforce, building on our $2.5M HRSA-funded Arizona Geriatric Workforce Enhancement Program (AZ-GWEP) grant (PI: Fain)
- Lead national, regional and local health care delivery policy for our seriously ill older adults
- Receive funding from the Home Centered Care Institute to build an academic “Institute of Excellence” in home care medicine at the UA
The Evidence Base for Home Care Medicine
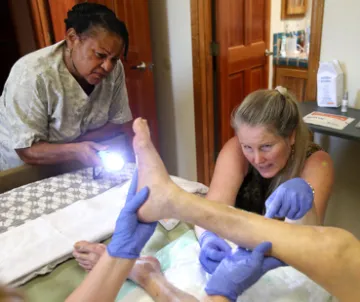
Home care medicine is highly innovative and disruptive care, bringing a redesigned “house calls” of yesteryear into the 21st century. It is not a quaint vestige of pre-war life, or a luxury for the wealthy. It provides extremely efficient and effective care for the growing number of older adults with serious illness and disability, and most often makes more medical and financial sense than a trip to the doctor’s office.
Why is home care medicine so important now? Our population is rapidly aging, and many older adults with severe chronic conditions and functional impairments have difficulty getting to the doctor’s office, forcing them to rely on the emergency room or hospital because of cognitive, physical and social barriers. They are increasingly isolated from the health care system, and suffer the consequences of highly fragmented care. And this poorly coordinated and unnecessary over-utilization is very expensive. These older frail adults comprise ~10% of Medicare beneficiaries, and yet disproportionately account for nearly 60% of Medicare costs.
The home care medicine team brings medical and social services into the home, assessing goals and needs, educating patients and families, treating chronic conditions, and in doing so reduces unnecessary emergency room visits and avoidable hospitalizations and readmissions, as well as the high associated costs. Families have a greater sense of security for their loved ones, and care provided is consistent with the patient’s and family’s wishes. The result is that older adults are able to remain at home, with dignity.
Over the past few years, during the same time that home care medicine has been gaining some momentum, emerging technologies expanded the care that could be provided safely and effectively in the home. Telehealth and telemedicine, body-worn sensors, bedside and remote diagnostics, and other technologies such as mobile imaging and ultrasound are just a few of the early advances that make it possible for home care medicine teams to provide ED and hospital-level care in the home. Vulnerable patients are then able to stay out of the ED and hospital, and avoid the known complications of hospital care, while benefiting from high quality care at lower costs in this “hospital without walls.”
There is no doubt — home care medicine is what we would all want for ourselves and our families – that comforting knock on the door when we are in need. We are now in the early stages of the development of home care medicine. There is so much work to be done: academic-community research in border and minority populations, development of bedside and remote diagnostic and therapeutic interventions through public-private/academic-industry partnerships, interprofessional education and training, workforce development, and health care policy, just to name a few. The University of Arizona is positioned to have a major impact locally, regionally and nationally.
Home Care Medicine - The Future
Help pass the bipartisan Independence at Home Act S.3130
We are building the world in which we are all going to grow old. Let’s do it right.

